News 4/24/12
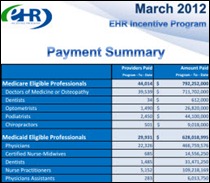
Through the end of March, the EHR Meaningful Use program paid Eligible Providers $1.4 billion in incentives. Of the 39,000 MDs or osteopaths receiving checks, 17,000 were specialists in family practice or internal medicine.
Cuyuna Regional Medical Center (MN) selects PatientKeeper technology to aggregate data from the MEDITECH system used by the hospital and the ambulatory care offices’ Allscripts system.
The US e-prescribing market is predicted to reach $205 million by 2017, which is far less than the $508 million forecasted for Europe for the same period.
Meritas Health Corporation (MO) chooses eClinicalWorks’ EHR for it 72 employed physicians. Meritas will interface eCW with its inpatient Cerner system, as well as LabCorp and Quest.
Wide River Technology Extension Center, Nebraska’s REC, announces that it has surpassed its goal of registering 1,000 primary care providers for its program. The REC has over 670 physicians live on EHRs and 145 have met Stage One MU requirements.
The 90-physician Allied Pediatrics (NY) selects Isabel Healthcare’s diagnosis decision support technology, which will be integrated with Allied’s EMR (GE Centricity I believe.)
Midwest Radiology Associates (OK) signs a long-term agreement with Affiliated Professional Services to provide billing and practice management services.
Brad Blakey, former VP of sales for NextGen, joins CareCloud as VP of sales.
Minnesota Eye Consultants selects the NextGen Ambulatory EHR for its 22 providers.
Lakeside Orthopedics (NE) contracts with SRS for EHR.
I am thrilled to announce simplifyMD as HIStalk Practice’s newest platinum sponsor. The six-year old company is based in Atlanta and offers an ONC-ATCB-certified EMR platform that’s been deployed by doctors in 27 specialties and thousands of end-users. The EHR is cloud-based, but practices also have the option to store data on a local server in their offices, just in case the Internet is temporarily unavailable. Unlike most traditional software vendors, simplifyMD offers a “pay as you go” option that can be discontinued at any time and costs a mere $395 per month. Last November the company announced it had secured $4.5 million in funding and named former McKesson SVP Mike Brozino as president. Founder Matt Ethington once sent me a photo of his very young son wearing some very red shoes, so I already had warm fuzzy feelings for this company. Many thanks for simplifyMD for supporting HIStalk Practice!
Every week I read new stories about medical office employees who are caught stealing thousands of dollars from their employers. This article, however, caught my eye because of the total lack of checks and balances in the practice. The Mandeville, LA woman, who has pled guilty of embezzling over $700,000 in less than four years, was in charge of payroll and over-compensated herself. She was also responsible for paying the plastic surgery practice’s American Express credit card and routinely used the card to cover personal expenses. Additionally she had access to the practice’s bank accounts and regularly transferred money to pay her rent and phone bills. Finally, she was the only employee authorized to make bank deposits and over time stole at least $60,000 in cash. Crazy.
2K Networking (PA) partners with gloStream to offer gloStream’s EMR solutions.























The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…