The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
News 11/4/10
Radiation Therapy Services, dba 21st Century Oncology, selects Sage Intergy for its 90 radiation therapy centers across 16 states.
The University of Wisconsin-Madison’s Center for Quality and Productivity Improvement takes a look at the effects of HIT tools on physician workflow in the outpatient setting, noting that previous studies have shown varied results. It’s a long read but here are a few conclusions worth noting:
- There is growing awareness that the analysis of workflow is necessary to ensure successful HIT implementation and to effect process improvement.
- When there’s a lack of integration of HIT into clinical workflow, quality and safety improvements suffer. HIT integration needs to support the cognitive work of the clinician and the workflows among organizations (e.g., between a clinic and community pharmacy), within a clinic, and within a visit.
- If HIT is to provide optimum performance, it must be designed to fit the specific context in which it will be used, specifically practice and patient types.
Core Solutions, which specializes in behavioral health software solutions, wins a contract to implement an EHR for 60 substance abuse providers affiliated with the Arkansas Office of Alcohol and Drug Abuse Prevention.
I’m glad the elections are over, along with the annoying political commercials and even more annoying phone calls. Over the next few weeks look for the lame-duck Congress to patch pending Medicare cuts before the 30% payment reductions kick in.
From the International Journal of Medical Engineering and Informatics: self-management of chronic disease can improve patient health and reduce hospital visits, and, PHRs and the use of the Internet have the potential to help patients better manage their diseases. Too bad no one wants to use PHRs.
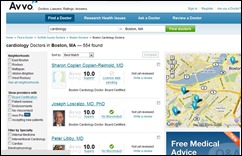
Start-up company Avvo announces it will expand its free online ranking services to include rankings of physicians. Avvo debuts with listings for over 800,000 doctors, drawn from public records and company research into doctors’ backgrounds and experience. Any predictions as to whether or not they’ll be able to filter out the retired/deceased/imprisoned physicians?
I happened upon this commentary by a couple of attorneys who specialize in negotiating HIT contracts between practices and vendors. They point out that one of the key services that RECs can provide is educating providers on HIT contracts, including some of the important provisions to minimize risk and to improve chances of achieving meaningful use:
RECs have the potential to serve as a valuable resource, especially for remote and underserved paper-based primary practices. However, RECs could be doing a disservice to physicians by failing to advise or provide them with essential EMR contract negotiation skills.
I was surfing YouTube today and noticed a recently posted series of videos highlighting a presentation by McKesson Sales National Sales VP Tammy Eden of the Physician Practice Solutions division. Each of the 10 clips are three to four minutes each and overview the final rules of the HITECH Act, the requirements for qualifying for Meaningful Use, and how to actually apply for reimbursement. The information is generic enough to be a great tool for anyone needing summary information, regardless of your EHR, and definitely worth a peek.




Inga,
Your three conclusions about the adverse effects of many HIT tools on physician workflow in the outpatient setting should be obvious to every clinician struggling with the cumbersome clinical data interfaces used by many EHR and HIE platforms.
All three can be directly applied to the management of the results of the billions of annual patient diagnostic tests that are indispensable in providing high value patient care and are a key component of all electronic health records. Some 70 to 80 percent of the data contained in a medical record consists of laboratory records and results, and approximately 70 percent of clinical decision-making is based on or assisted by laboratory test results. (1)
Unfortunately, there is a major nationwide problem with electronic test results reporting that has not yet become part of the public discussion. Billions of federal dollars have been legislated for “meaningful” EHR use, the creation of 62 RECs and 17 Beacon Communities, Comparative Effectiveness Research and the Nationwide-HIN. However, both public and private sectors have continued to overlook the adverse cost, quality and safety effects of the flawed processes used to report diagnostic test results to physicians and patients.
The continued use of infinitely variable reporting formats that display results as fragmented, incomplete data is a classic example of what Dr. Karyon and Dr. Karsh describe as “the lack of integration of health IT into clinical workflow in a way that supports the cognitive work of the clinician and the workflows within a visit, within a clinic and among different organizations.”
Fortunately, as President Reagan famously noted, “There are simple solutions, just no easy solutions.” EHRs (and HIE and PHR platforms) can maximize test results data liquidity and interoperability by replacing the variable reporting formats and their fragmented, hard to read data with a standard reporting format. Such an simple interface redesign can display clinically integrated, easily read and shared information and can reduce the number of screens by up to 80 percent.
Ideally, the growing emphasis on HIT system usability and costs, quality and patient safety, together with increasing HIT market competition and the emergence of collaborative care application platforms will produce a modular, vendor-neutral solution of the test results reporting problem. Finally meeting this unmet clinical need would be a good way to begin enhancing the overall workflow and productivity value of all future generations of EHR, HIE and PHR platforms and lowering their cost.
(1) http://www.chcf.org/publications/2010/01/electronic-release-of-clinical-laboratory-results-a-review-of-state-and-federal-policy