The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
News 3/13/14
From Harry C: “Re: CEHRT Hardship Exception Guidance. The move is not surprising given the number of vendors that are late releasing their Stage 2 versions, giving providers little time to get up to speed. Add in the fact that Stage 2 and ICD-10 must be implemented at the same time is too much for a lot of practices. The hardship will help practices that don’t have enough time to implement all the changes in workflow.” CMS revises its hardship exemption criteria to avoid 2015 Medicare payment penalties, allowing providers to indicate “2014 Vendor Issues” as the reason for the required exemption. I understand that providers are facing the perfect storm of deadlines but I find it ridiculous that CMS indicates it will rubber stamp hardship exemptions for any one that asks, rather than push back the official deadline.
Drchrono announces that its free EHR platform will be certified for MU Stage 2 “later this year.” Drchrono reports that over 60,000 medical professionals use its EHR platform. Given drchrono’s vague deadline for the release, I’m confident that a good number of drchrono physician users will be immediately jumping onto the CMS website to register their hardship exemption.
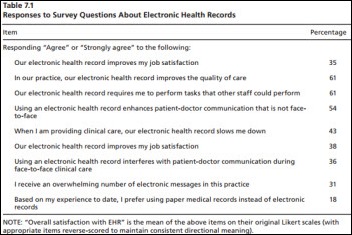
Physicians recognize the value of EHRs in concept and appreciate better access to remote patient information, but also believe EHRs undermine professional satisfaction and can negatively impact patient care. Those are some of the findings reported in a Rand Study on physician professional satisfaction based on data collected from 30 practices across six states. While less than one in five physicians would prefer to return to paper medical records, providers raised specific concerns about EHRs, including:
- Poor usability that doesn’t match clinical workflows
- Time-consuming data entry
- Interference with face-to-face patient care
- An overwhelming number of electronic messages and alerts
- The inability to exchange health information electronically with all providers
- The degradation of clinical documentation
- Expenses that were significantly higher than anticipated
The authors recommend that better EHR usability be an industry-wide priority and a precondition for EHR certification.
The ONC’s HIT Policy Committee releases preliminary Stage 3 MU recommendations, the majority of which are updates to objectives included in Stage 2. For example, Stage 2 requires providers to give at least 50 percent of patients to view their health information within four days of the information becoming available to the provider. Stage 3 requires providers to make the information available within 24 hours. The recommendations include 19 measures, which is two-thirds of the number included in initial Stage 3 proposals.
Qatar Foundation Primary Health Care Center becomes the first healthcare facility in the country to implement Cerner’s ambulatory EHR.
Greenway’s VP of industry and government affairs Justin Barnes participates in several recent White House summits, briefings, and panels to discuss HIT, patient engagement, privacy, the US economy, and related topics.
Not to take away from Barnes thought leadership and achievements but I was disappointed not to see a single female in the above picture.
University of Colorado Physicians goes live on the DocASAP self-scheduling system.
EClinicalWorks opens registration for its 2014 National User Conference, which runs October 17-20 in Orlando.
The EHR Association elects NextGen Healthcare CMO Sarah Corley to its executive committee.
E-MDs customer John Bender, MD of Miramont Family Medicine (CO) tells Medical Economics that his use of Lean management principles and use of IT have helped him to manage escalating costs and consistently grow the practice 45 percent.
A NIST report says that inadequate workflow integration forces users of ambulatory EHRs to develop system workarounds, suggesting that EHR vendors develop these capabilities:
- At-a-glance physician views of patient schedules
- Task reminders from previous patient visits
- Redacting and summarizing lab results
- Draft creation of patients orders in advance
- Conversion of working diagnoses to formal diagnoses
- Skip or defer tasks when workload requires
- Role-based views of progress notes
- Visually differentiate copied-and-pasted progress note text from newly entered documentation
- Manage referral and consultation messages with specialists
- Track scheduled consults and lab results review
Email Inga.






Inga, your observation (during Women’s History Month) about the lack of females in the picture above got me to thinking about the number of women who have served in Congress. According to History.House.gov, 298 women have served in the Senate and House of Representatives since 1917, when Representative Jeannette Rankin of Montana became the first woman to serve in Congress. I wonder how this number compares to the number of women in executive positions in other industries like healthcare.
As a grunt in the trenches user, it is somewhat surprising to me that anyone would need a formal report to know that “inadequate workflow integration forces users of ambulatory EHRs to develop system workarounds.”
Lawd, have mercy… I have looked for an EHR/EMR for years that “could learn to work around me rather than me having to learn to work around it.” I have never yet seen one where this is true. A few are closer than others, but every system I’ve ever encountered requires workarounds; most systems require a ton of them.
Where’s Dr. Chuck Webster (@wareflo) on this? He’s a workflow advocate from way back. Figured he’d be all over this NIST decree.
And, too, maybe Inga could interview Dr. Rick about his perspective on the NIST recommendations…?