News 8/18/11
The Big Lake Clinic (MN) will go live on Epic EMR September 1. The four-provider clinic is part of New River Medical Center and CentraCare Health System, both of which also run Epic.
Anesthesia Healthcare Partners, a provider of anesthesia practice management, hires RCM service provider MediRevv to provide A/R management services.
Declining reimbursements, competition for specialists, and the cost of technology contributed to the significant operating losses many provider organizations experienced last year. Physician compensation was relatively flat, with 70% of specialties seeing small increases in pay; overall compensation growth was about 2.4%.
Nuance Communications unveils Dragon Medical Practice Edition, which targets the needs of physicians in practices smaller than 25 providers. Nuance reports that the new edition yields a 15% improvement in accuracy over previous Dragon Medical releases and supports dictation directly into ambulatory EHRs.
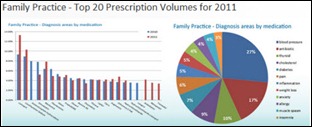
Medications for blood pressure, cholesterol, infection, and depression are the most commonly prescribed drugs by Practice Fusion users, according to the company’s Prescription Index report.
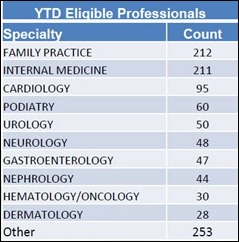
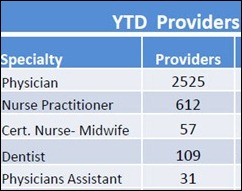
The above charts show the breakdowns for Meaningful Use payments to eligible providers, though the end of July. The Medicare figures (for a total of 1,078 total providers) break down the number of providers by specialty; Medicaid numbers (3,334 total providers) show recipients by provider type. More nifty facts can be found on the CMS website under “Provider Registration and Payments.”
In communities across the country, increasing numbers of physicians are moving from independent private practices to become employees of hospital systems. An Idaho paper reports on the trend in Boise, where Saint Alphonsus Health System added 19 doctors between September 2010 and June 2011. At St. Luke’s Health System, staff physicians were increased 50% after the hiring of about 100 doctors from June 2010 to June 2011. Physicians are making the move for a variety of reasons, including concerns about ongoing technology costs, fear of pending changes in reimbursement, and the desire to reduce the administrative tasks associated with running a private practice.
Things to add to your to do list: check out our sponsors offerings by giving their ads a click. They will appreciate your interest, as will I. Friend me on Facebook, connect with me on LinkedIn, and/or give me a follow on Twitter. If you want to make me really happy, send me an e-mail with interesting news updates, salacious rumors, or suggestions for Labor Day weekend getaways. And if you would like to fly me to the moon, share HIStalk Practice with a few industry folks who are not in the know. Thanks for reading.









The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…